As a first step toward diagnosis, your doctor discusses your personal history with you. Your nephrologist might ask questions about whether you've been diagnosed with high blood pressure, if you've taken a medication that might affect kidney function, if you've noticed changes in your urinary habits and whether you have family members who have kidney disease.
For kidney disease diagnosis, you might also need certain tests (blood, urine and imaging ) and possibly procedures to determine how severe your kidney disease is.
Some types of kidney disease can be treated, chronic kidney disease has no cure. Treatment usually consists of measures to help control symptoms, reduce complications, and slow progression of the disease. If your kidneys become severely damaged, you might need treatment for end-stage kidney disease.
Treating Complications
- Blood pressure medications. People with kidney disease can have worsening high blood pressure. Your doctor might recommend medications to lower your blood pressure.
- Medications to relieve swelling. People with chronic kidney disease often retain fluids. This can lead to swelling in the legs as well as high blood pressure.
- Medications to treat anemia. Sometimes with added iron, it can help produce more red blood cells. This might relieve fatigue and weakness associated with anemia.
- Medications to lower cholesterol levels. Your doctor might recommend medications to lower your cholesterol.
- Medications to protect your bones. Calcium and vitamin D supplements can help prevent weak bones and lower your risk of fracture. You might also take a phosphate binder to lower the amount of phosphate in your blood and protect your blood vessels from damage by calcium deposits.
- A lower protein diet to minimize waste products in your blood. Protein from food creates waste products that your kidneys must filter from your blood. To reduce the amount of work your kidneys must do, your doctor might recommend eating less protein.
Treatment for Kidney Failure
When you have kidney failure, your kidneys have stopped working well enough for you to live without treatment. There is no cure for kidney failure, but with treatment many people with kidney failure are able to keep doing activities they want or need to do. Talk to your provider about which treatment is best for you. Dialysis:
Dialysis:
Dialysis is a treatment that uses a machine to clean your blood. There are in-center dialysis locations and at home options that we discuss below.
Home Therapies
• Home Hemodialysis (Machine Dialysis at Home)
A NANI Vascular provider will place dialysis access in the body for blood to leave the body for cleaning. This treatment is used to filter wastes and water from your blood. This cleaned blood is then returned to the body through the same access.
If we have prepared for dialysis in advance, a surgeon creates dialysis access. They may put in something called a fistula or graft. A fistula is when the surgeon creates dialysis access using the blood vessels in the body. A graft is when the surgeon creates a dialysis access by implanting synthetic tubing in the body. These options take about six weeks to mature. The access sometimes is a catheter in an emergency.
Home hemodialysis means doing hemodialysis at home. Doing home hemodialysis means getting to dialyze more often. Patients often dialyze four to five days a week and sometimes even daily. Because of more frequent dialysis, patients feel better. This mode of treatment requires several weeks of training.
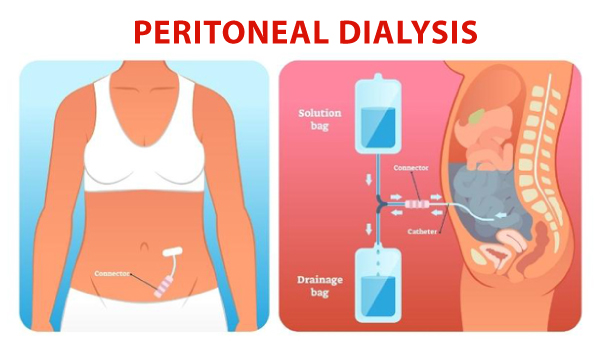
• Peritoneal Dialysis
Peritoneal dialysis, or PD, is a way to remove waste products from your blood when
your kidneys can no longer do the job adequately. The treatment uses the inner lining
of your belly (peritoneum) as a filter.
A sterile fluid flows through a tube into part of your abdomen and filters waste from
your blood. While you go about your day, the fluid will collect wastes and water.
Later, the fluid with filtered waste is removed from your abdomen and discarded.
Unlike hemodialysis in a center, you can give yourself peritoneal dialysis treatments
at home, at work or while traveling.
If you are a candidate for PD home dialysis, you’ll have a special catheter put in
with an outpatient procedure. NANI Vascular has a team in place that can help
you with this procedure. Then, you will go to two weeks of training with an
experienced PD nurse to learn all you need to know to do PD at home. Once you
are done with training, you will only go to the clinic about once each month for a
blood test and to meet with your care team, which will include your physician,
nurse, nutritionist and social worker.
Someone from your care team will be available 24 hours a day, if you ever need help.
In-Center Treatments
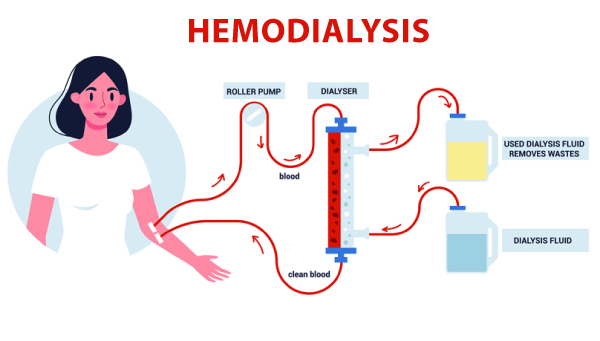
• Hemodialysis (Machine Dialysis at a Facility)
Similar to home hemodialysis, NANI Vascular provider will place dialysis access in the patient's body for blood to leave the body for cleaning. The blood then goes to a filter on a machine where the cleaning occurs. This cleaned blood is then returned to the body through the same access.
Patients will dialyze 3 days a week. Some patients can dialyze less often, including twice or even once a week, your doctor will discuss the best option for you.
This is a good modality for patients who cannot take care of themselves or live in a nursing home. A downside is that the patient will have to arrange his or her life around their dialysis schedule.
The dialysis unit can arrange patient transportation to and from the dialysis unit.
KIDNEY TRANPLANT & CONSERVATIVE MANAGEMENT
 Kidney transplant
Kidney transplant
A kidney transplant is a surgery to give you a healthy kidney from a donor. Transplanted kidneys can come from deceased or living donors. The healthy kidney can do the job that your kidneys did when they were healthy. A kidney transplant is not a cure, but a treatment for kidney failure. You will need to take medicines and take special care of your transplanted kidney for the rest of your life to keep your body from rejecting the new organ.
 Conservative Management
Conservative Management
For some who choose not to have dialysis or a kidney transplant, a third option is to treat your kidney failure with conservative measures. Conservative measures likely will include symptom management, advance care planning and care to keep you comfortable. This allows them to focus on improved quality of life.
